 Researchers from the North Carolina State University and the University of North Carolina at Chapel Hill have developed a patch designed to monitor a patient’s blood and release blood-thinning drugs to prevent dangerous blood clots, or thrombosis. The team’s work was published in Advanced Materials.
Researchers from the North Carolina State University and the University of North Carolina at Chapel Hill have developed a patch designed to monitor a patient’s blood and release blood-thinning drugs to prevent dangerous blood clots, or thrombosis. The team’s work was published in Advanced Materials.
When blood clots disrupt the flow of blood throughout the body, the result can cause pulmonary embolism, heart attack or stroke. Conventional treatment requires patients to regularly test their blood to ensure proper dosages of blood thinners such as Heparin.
If a patient uses too small a dose, it may not prevent a relapse of thrombosis. On the contrary, too large a dose can cause spontaneous hemorrhaging.
“Our goal was to generate a patch that can monitor a patient’s blood and release additional drugs when necessary; effectively, a self-regulating system,” co-corresponding author Zhen Gu said in prepared remarks.
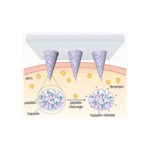
The smart patch includes polymeric microneedles that are made up of hyaluronic acid and Heparin. The modified polymer is responsive to an enzyme, thrombin, that sparks clotting in the blood.
“The more thrombin there is in the bloodstream, the more Heparin is needed to reduce clotting,” co-lead author Yuqi Zhang explained. “So we created a disposable patch in which the more thrombin there is in the blood stream, the more Heparin is released.”
“We will further enhance the loading amount of drug in the patch. The amount of Heparin in a patch can be tailored to a patient’s specific needs and replaced daily, or less often, as needed,” co-lead author Jicheng Yu added. “But the amount of Heparin being released into the patient at any given moment will be determined by the thrombin levels in the patient’s blood.”
The team tested its smart patch using a mouse model in which subjects were injected with fatal doses of thrombin to initiate blood clotting in the lungs. In the 1st experiment, mice were either untreated, given a shot of the blood thinner Heparin or given the smart patch. The mice were injected with thrombin and 15 minutes after the injection, only the mice that were untreated died.
In the 2nd experiment, the thrombin was injected 6 hours after treatment with Heparin or the smart patch. After 15 minutes, all of the mice with the smart patch had survived and 80% of the mice that received Heparin had died.
“We’re excited about the possibility of using a closed-loop, self-regulating smart patch to help treat a condition that affects thousands of people every year, while hopefully also driving down treatment costs,” Gu said. “This paper represents a good first step, and we’re now looking for funding to perform additional preclinical testing.”

